Get the latest news delivered right to your email.
2024 Election
Top Stories
Advertisement
'Shrek 2' Re-Release Embarrasses Disney, Performs Better Than All These New Animated Films
The 20th anniversary re-release of "Shrek 2" just completed its opening weekend at the box office, passing up the totals of some newer films.
By Michael Austin
April 16, 2024
Comment
MoreShare
Arrest Warrant Issued for Democrat After Going on Drunk Rant, Threatening to Shut Down Local Bar
A Democratic state legislator in Pennsyvania who was videoed two months ago raving in a bar is in even deeper trouble now.
By Jack Davis
April 16, 2024
Comment
MoreShare
Trump Couldn't Help but Smile, Nod Along at Potential Juror's Response to Question
Day 2 of jury selection in former President Donald Trump's 'hush money' trial led to Trump flashing a smile and getting a warning.
By Jack Davis
April 16, 2024
Comment
MoreShare
Patrick Mahomes Refuses to Call for Gun Control After Kansas City Shooting - 'I Continue to Educate Myself'
The star quarterback is steering clear of partisan messaging on one of the most hotly debated topics in American politics.
By Richard Moorhead
April 16, 2024
Comment
MoreShare
Watch: Stephen A. Smith Lights Up Democrats Going After Trump - 'You're Scared You Can't Beat Him'
Stephen A. Smith took to his Youtube channel to blast the politicized trial of former President Donald Trump.
By Samuel Short
April 16, 2024
Comment
MoreShare
'Unbiased' CNN Reporter Gets Wake-Up Call from Normal Americans When He Can't Imagine Why Anyone Would Miss Trump Years
A CNN commentator turns to armchair psychology to try to understand Americans -- and remembers a college ex-girlfriend.
By Joe Saunders
April 16, 2024
Comment
MoreShare
Pro-Palestinian Agitators Attempting to Block Miami Road Find Out Things Are Different in Florida
Miami police removed pro-Palestinian protesters who blocked traffic in yet another show of characteristic left-wing narcissism.
By Michael Schwarz
April 16, 2024
Comment
MoreShare
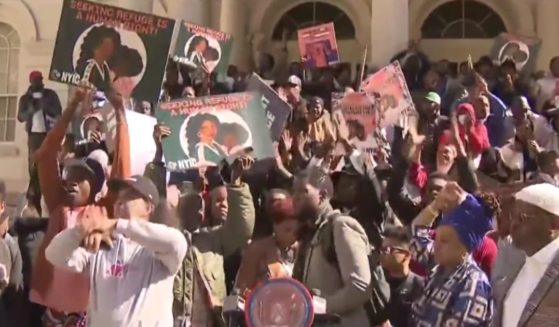
Hundreds of African Immigrants Flock to NY City Hall to Complain That Living Conditions Are 'Not What They Were Expecting'
Migrants from Africa and elsewhere protested NYC living conditions, prompting self-righteous liberals to respond with more virtue-signaling.
By Michael Schwarz
April 16, 2024
Comment
MoreShare
Advertisement
Bidenomics: Americans Taking Drastic Measures to Keep a Roof Over Their Heads, Poll Shows
Joe Biden's economy is so bad that some Americans report having to skip meals in order to remain afloat.
Comment
MoreShare
Bible Prophecy: What Do Israel's Mysterious Red Cows Have to Do with Middle East Tensions and End Times?
Red heifers delivered from Texas to Israel may well be another sign that the world is entering the end times.
Comment
MoreShare
The True Jesus: Dispelling the Liberal Myths and Misperceptions - Part Three
Christians can and should fight the culture war; we simply need to understand God’s rules of engagement first.
Comment
MoreShare
Advertisement